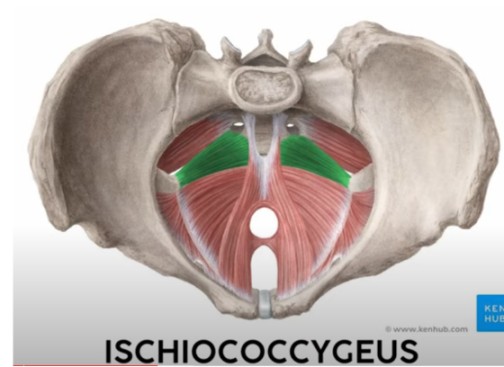
THE MENSTRUAL CYCLE
The menstrual cycle is a sequence of events that occurs every 21-36 days in females after puberty, continuing throughout the childbearing years.
Factors that Influence the Menstrual Cycle
For a normal menstrual cycle to occur, the following components must be functioning properly:
- The Hypothalamus: Stimulates the release of luteinizing hormone-releasing hormone (LHRH), which triggers the pituitary gland.
- The Pituitary Gland: Secretes hormones that stimulate the ovaries.
- The Ovaries: Produce hormones that trigger changes in the uterus and the growth of the ovum.
- The Uterus: Experiences changes, shedding the endometrium regularly.
- The Vagina: Acts as a passageway for menstrual flow.
- Hormones: Key players in regulating the menstrual cycle and causing various changes.
Hormones Involved in the Menstrual Cycle
(a) Gonadotrophic Hormones: The hypothalamus, part of the diencephalon located in front of the thalamus, secretes gonadotropin-releasing hormone (GnRH), which stimulates the anterior pituitary gland to release follicle-stimulating hormone (FSH).
Functions of FSH:
- Promotes the maturation of ovarian follicles (Graafian follicles), usually one at a time, and triggers estrogen secretion, leading to ovulation.
- The developing follicle secretes estrogen, causing the uterus to proliferate and the breasts to enlarge, preparing for breastfeeding.
- About 24-36 hours before ovulation, the anterior pituitary gland secretes luteinizing hormone (LH), causing the Graafian follicle to rupture, leading to ovulation and the formation of the corpus luteum.
- The corpus luteum secretes progesterone, which thickens the endometrium and maintains pregnancy.
Note:
- If fertilization doesn’t occur, progesterone withdrawal happens.
- The corpus luteum degenerates into the corpus albicans (a white body) and finally becomes fibrous.
- The cycle then begins again due to stimulation by the hypothalamus.
(b) Ovarian Hormones.
1. Oestrogen:
- Produced by growing follicles (granulosa cells and theca).
- Responsible for the development of female secondary sexual characteristics (e.g., breast growth).
- Causes proliferation of the endometrium, prepares the vagina, and promotes the production of cervical mucus.
2. Progesterone:
- After ovulation, LH stimulates the corpus luteum to produce high levels of progesterone and low levels of estrogen.
- Progesterone causes the endometrium to become more tortuous, raises basal body temperature, and induces sensations of fullness in the breasts before menstruation.
- The rise in ovarian hormones decreases the flow of GnRH, leading to reduced production of FSH and LH. This is a negative feedback loop.
- A positive feedback mechanism occurs when blood estrogen levels rise, stimulating the hypothalamus to secrete more luteinizing hormone-releasing factor.
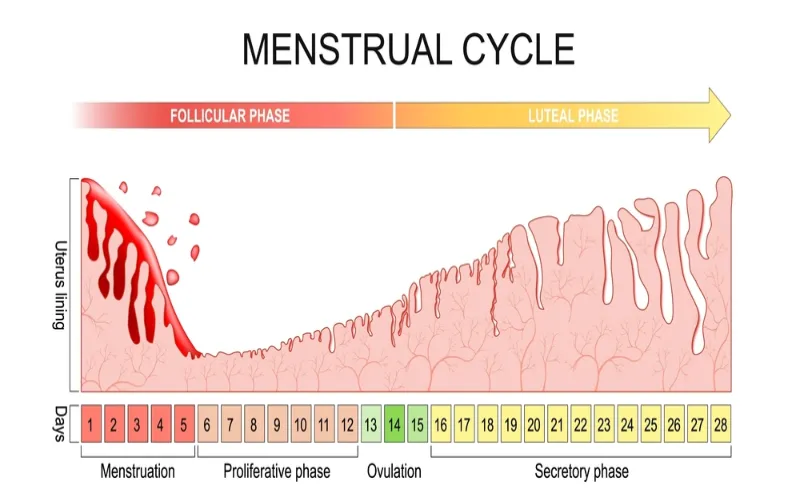
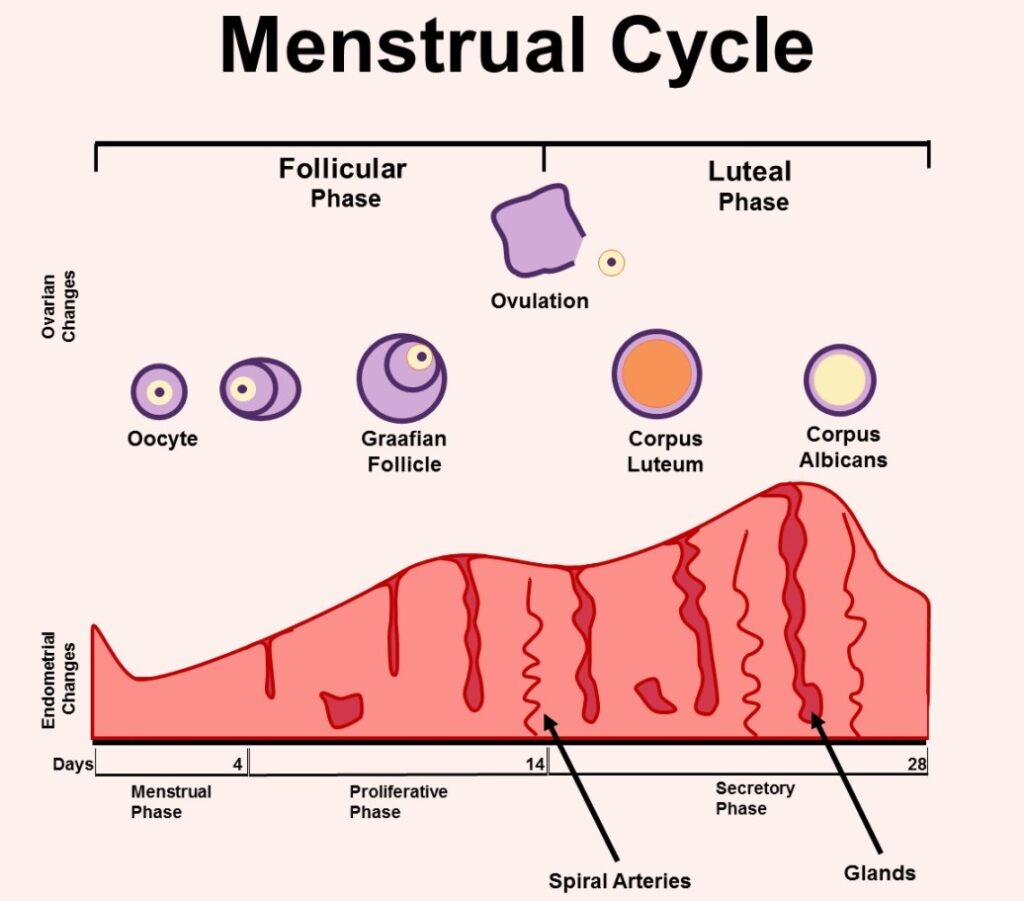
Uterine Phases/Events of the Menstrual or Endometrial Cycle
1. Menstrual Phase.
- If the ovum is not fertilized, the corpus luteum degenerates, causing progesterone and estrogen levels to fall.
- The functional layer of the endometrium, which relies on high levels of ovarian hormones, is shed during menstruation.
- High circulating levels of progesterone and estrogen inhibit FSH and LH production in the anterior pituitary gland. If pregnancy occurs, these hormones prevent the release of another ovum.
- When the corpus luteum degenerates, falling hormone levels cause the anterior pituitary to resume FSH secretion, initiating the next cycle.
2. Proliferative Phase
- This phase begins immediately after the menstrual phase and lasts until ovulation. It coincides with the follicular phase.
- The endometrium regenerates, forming a new layer.
- This phase typically lasts 10 days in a 28-day cycle:
- Early proliferative phase: Occurs 4-7 days after menstruation.
- Mid proliferative phase: Occurs 8-10 days after menstruation.
- Late proliferative phase: Occurs 11-14 days after menstruation.
- FSH stimulates the growth and maturation of Graafian follicles, which produce estrogen to repair the endometrium.
- The endometrium thickens, consisting of three layers:
- Basal layer: Next to the myometrium, not shed during menstruation, as it contains the necessary structures to rebuild the endometrium.
- Functional layer: Spongy, tubular glands, about 2.5 cm thick.
- Compact layer: Cuboidal ciliated epithelium.
Note: The functional and compact layers (b and c) are shed during menstruation.
3. Secretory Phase
- This phase follows the proliferative phase and is regulated by progesterone.
- The endometrium becomes edematous (thickens and swells) and develops a spongy appearance.
- Secretory glands produce increased amounts of glycogen to nourish a potential fertilized ovum.
- This phase lasts for about 14 days.
Note:
- If the ovum is not fertilized, menstruation begins, marking the start of a new cycle.
- If the ovum is fertilized, the zygote travels to the uterus and becomes embedded in the endometrium, producing human chorionic gonadotropin (HCG). This hormone supports the corpus luteum, ensuring continuous secretion of progesterone and estrogen to maintain pregnancy.
- After about 12 weeks, the placenta forms and takes over hormone production (estrogen, progesterone, and gonadotropins) to sustain the pregnancy.
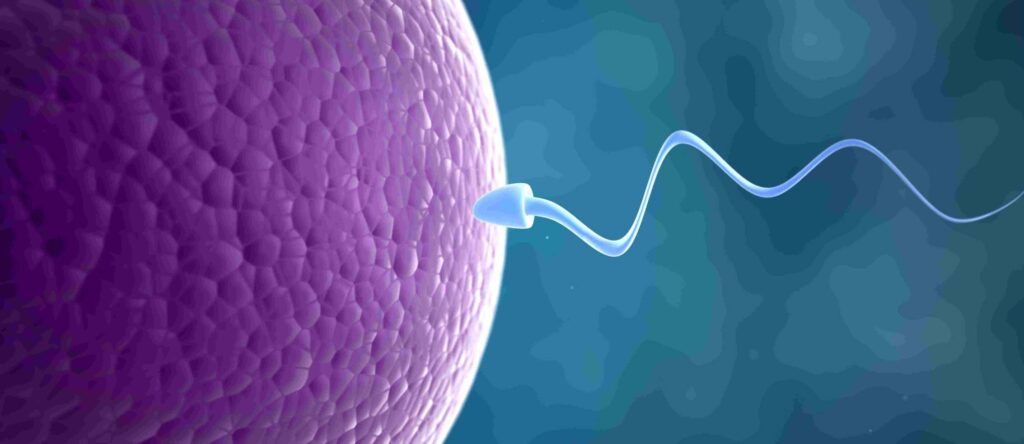
Gametogenesis
Gametogenesis is the developmental process that leads to the creation of reproductive cells.
Before fertilisation, gametes have to be formed in the process of gametogenesis which takes place on the principles of meiosis.
Production of a Mature Ovum (Oogenesis)
Oogenesis is accomplished through meiosis, a process beginning during embryonic development.
A primary oocyte produces one secondary oocyte and a polar body.
The secondary oocyte and the first polar body then give rise to a mature ovum and three polar bodies, which degenerate. The ovum is the largest cell in the body.
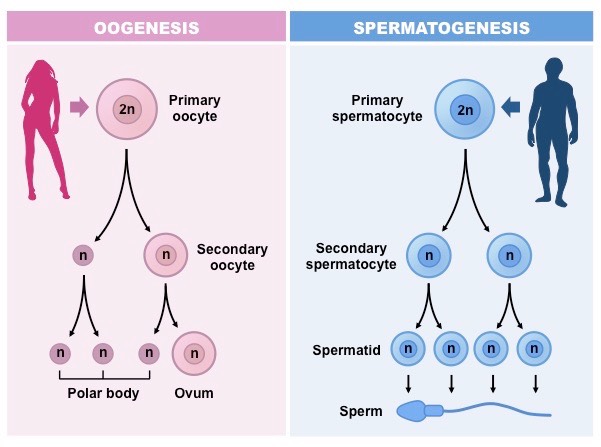
Spermatogenesis (Production of Sperm)
Spermatogenesis, the formation of spermatozoa, begins at puberty (around 14-16 years). Sperms are produced in the basal layer of the germinal epithelium of the testes under the influence of Follicle-Stimulating Hormone (FSH). This occurs through meiotic cell division.
- Primitive structures (spermatogonia) in the testes are nourished by Sertoli cells, developing into primary spermatocytes. These primary spermatocytes, possessing a diploid number of chromosomes, undergo meiosis to form two daughter cells: secondary spermatocytes.
- The Luteinizing Hormone (LH) acts on the secondary spermatocytes, initiating the second meiotic division and forming spermatids. The larger portion of the spermatid develops into a spermatozoon (sperm). This transformation of spermatids into spermatozoa is called spermiogenesis.
The spermatozoon has three main parts:
- Head: Contains the acrosome (with the hyaluronidase enzyme, which breaks down the ovum’s outer layer for sperm entry) and the nucleus (containing chromosomes and genetic material).
- Body (Midpiece): Provides nutrients for the sperm.
- Tail (Flagellum): Propels the sperm after ejaculation.
Male Hormones:
- The hypothalamus produces gonadotropin-releasing factor (GnRH), which stimulates the anterior pituitary gland.
- FSH acts on the seminiferous tubules to stimulate spermatozoa production.
- LH stimulates interstitial cells to produce testosterone, the primary male sex hormone responsible for the development of secondary sexual characteristics in boys at puberty, including:
- Increased muscle growth and height/weight gain.
- Enlargement of the larynx (deeper voice).
- Growth of hair on the face, armpits, chest, abdomen, and pubic area.
- Enlargement of the penis, scrotum, and prostate gland
Revision Questions:
- Define meiosis.
- Describe the formation of a mature ovum.
- State the differences between a primary and a secondary oocyte.
- What is spermiogenesis?
- State two functions of the testes.
- Describe the male reproductive system.
- List three hormones that influence spermatogenesis.
- List three hormones involved in male reproduction.
Menstruation Cycle Read More »